What does urinary incontinence mean?
It is the involuntary, i.e. without our will, loss of urine to such an extent that causes a hygiene problem (dermatitis) or a problem of social acceptance (smells, wet clothes, etc.). It is a symptom, a clinical manifestation and not a disease.
Is urinary incontinence a common problem and at what ages does it occur?
Incontinence concerns all ages, occurs in children and young people, but is particularly common in old age. Women are more affected — in America 10,000,000 people suffer from urinary incontinence and 85% are women. It is estimated that one in four women aged 30–59 has experienced at least one episode of urinary incontinence.
The condition is accompanied by significant morbidity, which includes placement of indwelling catheters, urinary tract infections, pressure sores, etc. It also causes mental disorders, depression, isolation, and anxiety, while we should not overlook the sexual dysfunction it causes, especially in younger people.
A major part of the problem is ignorance around it. About half of patients have never consulted a doctor about their problem, and non-specialists rarely ask or reveal the symptom of incontinence. Additionally, women suffering from urinary incontinence hesitate to confide in their problem even to the doctor because they feel ashamed.
What causes urinary incontinence?
A wide range of conditions and disorders can cause urinary incontinence, such as genetic abnormalities, surgeries, injuries to the pelvis and spine, neurological diseases, inflammation, urinary tract infections, and aging. Additionally, incontinence can occur as a result of childbirth.
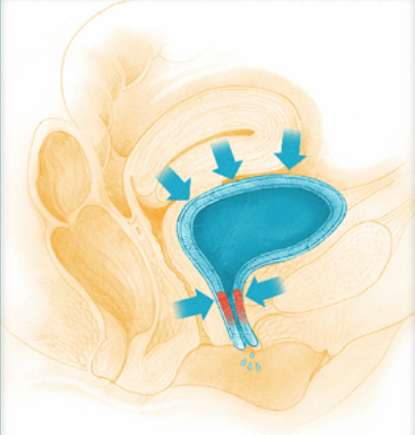
Incontinence is a problem of the urinary system, which consists of two kidneys, two ureters, a bladder, and a urethra. Urine is produced in the kidneys after filtering the blood and is a waste product that the body excretes. From the kidneys, urine descends to the bladder through the ureters (two muscular tubes that connect the kidneys to the bladder), where it is stored. The bladder is surrounded by a muscle called the detrusor, which relaxes as the bladder fills with urine, up to about 500 cc, while the bladder neck remains closed to prevent urine loss.
When the brain determines it is convenient to empty the bladder, it signals the bladder to contract. If not, it instructs the bladder to wait, allowing it to continue storing urine while the bladder neck valve remains closed. Once the appropriate conditions arise, the brain commands the sphincter of the bladder to open, causing the bladder to contract and urine to exit through the urethra.
The sphincter, a muscle that encircles the urethra, controls its activity. Therefore, if any part of the urinary system described above exhibits abnormalities, it may result in incontinence.
Types of urinary incontinence
Stress Incontinence
The muscles surrounding the neck of the bladder relax and the bladder can no longer cope with great pressures. Activities that increase pressure in the abdomen, such as sneezing, coughing or standing, cause urine loss. It is the type of incontinence that usually occurs after childbirth.
Urge Incontinence
The sudden urge to urinate, but without enough time to hold on until reaching the toilet. At that moment the bladder contracts involuntarily, the valve (the neck of the bladder) opens and urine is expelled. This may be due to a neurological condition but many times no cause is found and it is called idiopathic unstable (or more correctly overactive) bladder.
Mixed Incontinence
The combination of the above two types.
Incontinence can also occur after a surgery such as a hysterectomy, a cesarean section, a prostatectomy or even after a bowel operation.
Reflex Incontinence
When the bladder fills, it sends a signal to the brain. The nerves that carry this message can be damaged, and the message never reaches the brain. The bladder will empty on its own without our willing it, and in this case we will not understand in advance that we want to go to the toilet.
Incontinence Due to Overfilling
This may be a result of urinary retention. Just like a balloon that we fill with water — when it fills up and no longer fits, it starts to overflow — the bladder fills up and slowly some drops leave, or there is a constant loss of urine.
Can incontinence in men be cured?
Although incontinence in men is due to different causes than in women, the treatment options are similar and every day they become more known and available. Radical prostatectomy — surgical removal for prostate cancer — is the leading cause of urinary incontinence in men. 40% of men report incontinence a few weeks after prostate removal. Most of them can regain control of their urination, but some will not. A large clinical research published in January 2000 in the Journal of the American Medical Association reported that 8.4% of men after prostatectomy experienced incontinence 18 months after surgery.
The problem is what we call sphincter insufficiency — the sphincter is not strong enough to withstand the abdominal pressure exerted when someone coughs or sneezes, resulting in loss of urine. The sphincter is a "ring" of muscles that controls the opening of the urethra. When incontinence is diagnosed, doctors may recommend a series of non-invasive treatments until the sphincter regains strength, including exercises, collagen injections and external devices.
The Artificial Sphincter
For the last 30 years, the Artificial Sphincter has been the most proven surgical solution. This tiny device is the result of advanced engineering and medical research and mimics the function of the normal sphincter, which controls the flow of urine. The Artificial Sphincter is placed entirely inside the body and allows direct and discreet control of urination.
Its operation is based on the sequential filling and emptying of a tiny, flexible "ring" that surrounds the urethra. When the "ring" is filled with fluid, it keeps the urethra closed. When fluid is transferred to a reservoir located in the lower part of the abdomen, the "ring" relaxes around the urethra, allowing urine to pass through.
According to published studies, the satisfaction rate of patients after artificial sphincter placement exceeds 90%, and 96% of them would recommend it to a friend with a similar problem. This method has been applied worldwide for 30 years to about 90,000 men. In Greece, this method has been applied for the last 15 years with very high success rates.
Urethral Support Tape
For cases with mild to moderate incontinence or when the patient cannot handle the artificial sphincter, the placement of a urethral support tape is a new, very reliable solution. Most patients are continent immediately after surgery and can return to their normal activities within a few days. According to published studies, the satisfaction rate of patients after the placement of urethral support tape approaches 90%. The tape is placed with a simple operation in less than 1 hour, with a one-day hospitalisation.
What is the treatment of incontinence?
There are three broad categories: behavioral, pharmaceutical and surgical.
Behavioral Therapy
-
Scheduling urination:
The patient goes to the toilet at a specific time by the clock, every 2–4 hours regardless of whether they want to urinate or not. The goal is to keep the patient dry and is indicated for elderly people with incontinence, children with nocturnal enuresis and Alzheimer's disease sufferers.
-
Reeducation of the bladder:
The patient also goes at scheduled times to urinate, but the interval between one urination and another gradually increases, so the bladder learns to delay urination for longer breaks. This technique is applied to urge and mixed type incontinence.
-
Pelvic floor exercises:
Exercises of the muscles of the pelvis, vaginal cones, etc. can be combined with biofeedback therapy and are usually recommended in stress incontinence.
Drug Therapy
There is a category of drugs called anticholinergics that aim to treat mainly urge incontinence. Because these drugs interact with other drugs that someone may take, especially the elderly, we should avoid taking them on our own and definitely have them recommended by a doctor. For the treatment of stress incontinence in women, a medication from the class of serotonin inhibitors (duloxetine) has shown very encouraging first results.
Surgical Treatment
The surgical treatment is performed after the Urologist has made a diligent and correct diagnosis for the type of incontinence. There are many techniques used mainly to treat stress incontinence and incontinence due to sphincter damage after prostatectomy, such as bladder neck suspension, injections around the urethra with collagen and other inert materials, and the artificial sphincter as mentioned above — a device placed around the urethra and handled externally by the patient, with great results under the hands of experienced urologists.
10 warning signs to visit your doctor
- • Loss of urine that prevents you in daily activities.
- • Loss of urine that causes embarrassment.
- • Loss of urine after an operation such as hysterectomy, caesarean section, prostatectomy, etc.
- • Weakness or difficulty urinating.
- • Urinating more often than before without having any obvious urinary tract infection.
- • Feeling like running to the toilet and not being able to postpone it — even until getting there, some urine losses occur.
- • Pain in the bladder area or pain when urinating.
- • Frequent urinary tract infections.
- • Progressive reduction of the urine stream with or without the feeling that the bladder does not empty completely after each urination.
- • Abnormalities in urination after a neurological condition such as a stroke or multiple sclerosis.
Contents
Book an Appointment
Dr. Mertziotis specialises in the diagnosis and surgical treatment of urinary incontinence, including artificial sphincter placement and urethral support tape.
Book an Appointment Online +30 210 6465359 Ελληνικά
Ελληνικά